I am a Survivor: The Devastation of Healthcare-Associated Infections

My name is Mary Millard, and I am a patient who lives with a chronic healthcare-associated infection (HAI). This is my story.
Up until the fall of 2014, I was a healthy 55-year-old with an exceptional life. I enjoyed playing beach volleyball, running with my dog, and hiking in the Blue Ridge Mountains when I wasn’t busy obtaining my graduate degree in education.
One day and out of the blue, I started having small bouts of rapid heartbeats and sought medical care. A cardiologist prescribed medication to help regulate the rate. Because I was very healthy and only in my mid-fifties, I was sure the medication would help. Unfortunately, it did not.
Going to the hospital
On a particularly bad day, when my heart felt like it was going to jump out of my chest and indigestion seemed to be at its worst, my husband and I decided it was time to seek emergency treatment at a nearby hospital.
Both of us were consumed with fear and uncertainty as the medical staff tended to me. I was hooked up to monitors, my blood drawn, and had a CT scan. Eventually, I was given a diagnosis. I had a 6.3cm ascending aortic aneurysm and a partially collapsed aortic valve. The cardiothoracic surgeon said it was a genetic issue, as there were no underlying diseases or health issues. I was admitted for an aneurysm repair and valve replacement surgery.
An unexpected collapse
The day before the surgery, my aortic valve collapsed completely. I went into cardiac arrest.
I remember a sudden feeling, like a dagger was being thrust into my chest, doubling me over in pain. It happened again and again as I lunged towards the bed to hit the call button, all the while screaming in excruciating pain. I remember a flurry of white coats surrounding me. I remember seeing my husband standing with a confused look in the doorway and holding a folder that contained our pet pictures so that my patient room could be more comforting for me. The last thing I remember is being held down on the CT table and told not to breathe.
I only know what happened after the CT room from seeing my medical records and hearing the accounts as told by my doctors, PAs, and my husband.
They took me to the Cath lab on my floor because they feared my aneurysm had burst. When I was placed on the table, a code blue was roared. My heart had stopped. A cardiologist tried the paddles three times, but no luck. My code lasted 6 minutes and 45 seconds as they scrambled to get life support equipment together.
I was attached to an extracorporeal membrane oxygenation (ECMO) machine. This is a life-support machine that circulates and oxygenates your blood while an external pacemaker beats your heart.
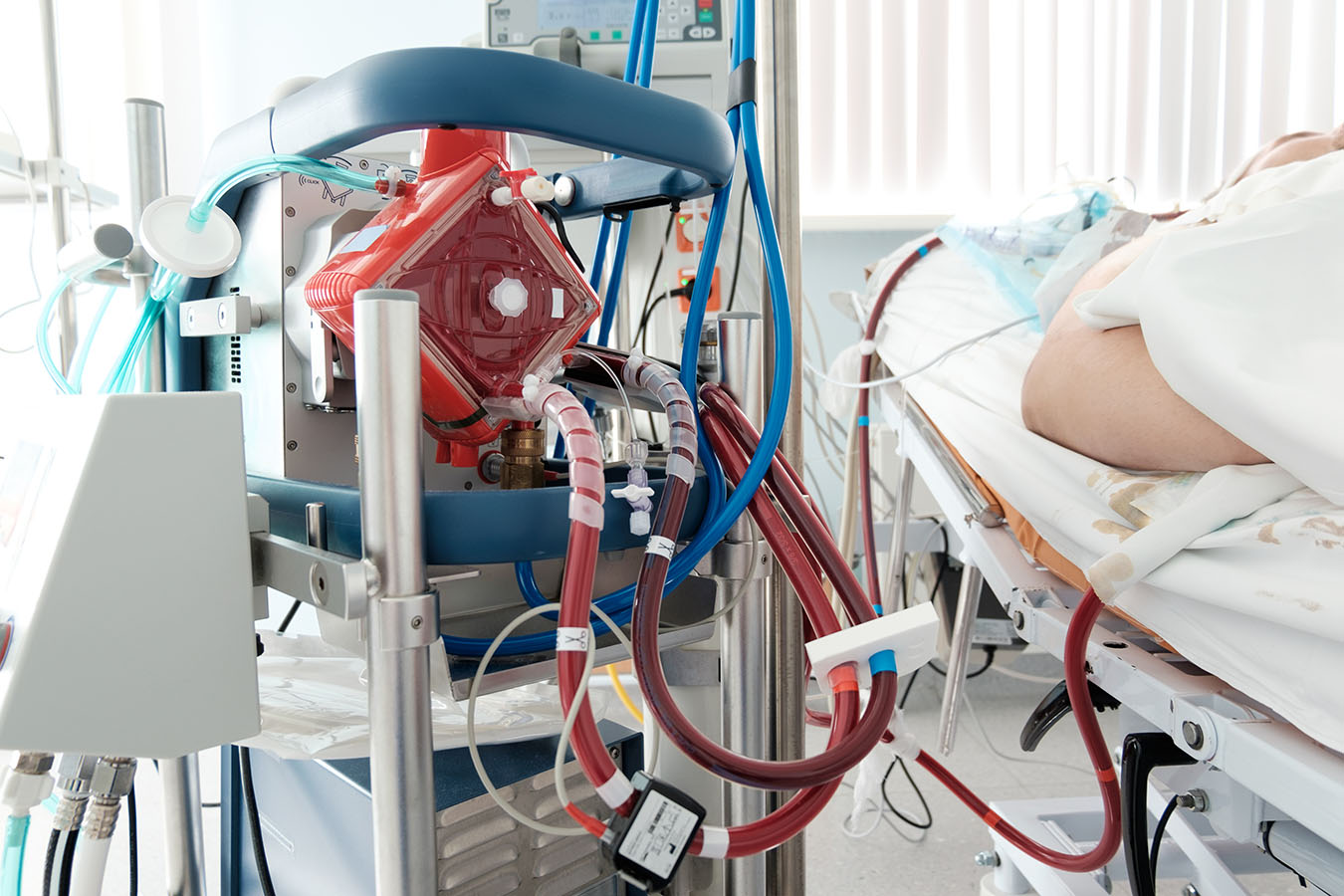
ECMO machine
According to my husband (who was there every day), the ECMO was in place for three days. On the fourth day, the nurse informed him my heart had started beating on its own! He thought, “this is finally over,” and felt immense relief that my surgery was finally coming.
Open heart surgery
Because the doctors feared the aortic aneurysm would burst, my surgery was rescheduled for two weeks later. To help with my recovery so I could undergo surgery, they kept me in a medically-induced coma.
According to my frightening medical notes, my white blood cell count was off the charts even before surgery, but this was explained as normal and blamed on the ECMO. Things went smoothly and quickly. Within hours I was in recovery in the ICU.
Four days after the surgery, I was placed in step-down with the possibility of going home soon. On the fifth day, my husband noticed that I was speaking in a confused manner, was feverish, and could not hold my head up. A stroke code was called, and a six-hour neurology workup was ordered.
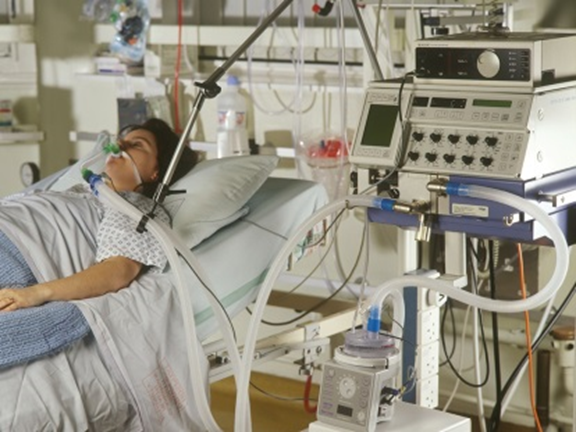
Photo taken by Mary’s husband in the ICU during septic shock
Septic shock reveals the HAI
It was not a stroke. I was in acute septic shock and was rushed back to the ICU. My groin wound was red and not healing. Something was wrong. Wound cultures showed that I had contracted Pseudomonas aeruginosa, a bacterial infection.
It was a healthcare-associated infection. The entry point of the infection was in the left groin wound, where I had been connected to the ECMO machine. I learned about how this happened later, from my infectious diseases doctor.
The contaminated surface
An ECMO cannula for blood flow had been placed in my groin and in my jugular. When the cannula packet was unsheathed, it was laid on a nearby counter next to the sink for only a few seconds. Just seconds. But long enough for some water left on the counter – sink splash – containing Pseudomonas bacteria to contaminate the surface of the cannula and, later, my body.
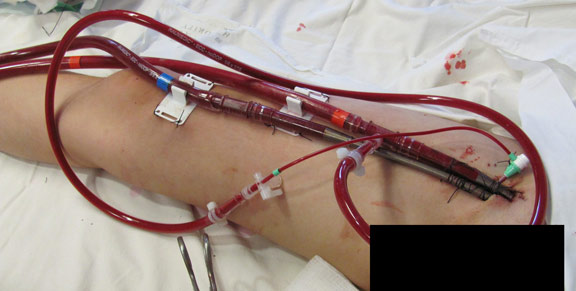
The ECMO cannula insertion site
Pseudomonas is a gram-negative bacterium that creates a sticky biofilm on surfaces. It resides in this biofilm on my graft, valve replacement, tricuspid valve ring, and groin graft (from the ECMO cannula). Because of increasing antibiotic resistance, it is also a multi-drug resistant (MDR) bacteria.
Pseudomonas loves damp, dark places and sink traps are ideal living quarters. Surfaces contaminated with such bacterial biofilms are extremely dangerous, as they are difficult to disinfect properly.
The aftermath
After a week of duo antibiotic therapy with Tobramycin and Cefepime, it was decided to reopen my sternum so the surgeon could attempt to clean out the chest cavity from infection residue, debride the aortic graft to attempt a biofilm removal, and perform an Omental flap procedure (where they take part of the tissue from your abdomen to place in your chest cavity to nourish for healing).
My chest cavity debridement procedure
A slow and painful recovery
Recovery was slow, and I was kept in another medically-induced coma to help. Once I was brought around, I had already spent 55 days in the hospital. This was bittersweet because it brought crippling fear and confusion. I still had no concept of date or time at this point, and the feeling of dread was deep as I became more aware of what had transpired. I also realized with dread that my legs would not work. I could not stand.
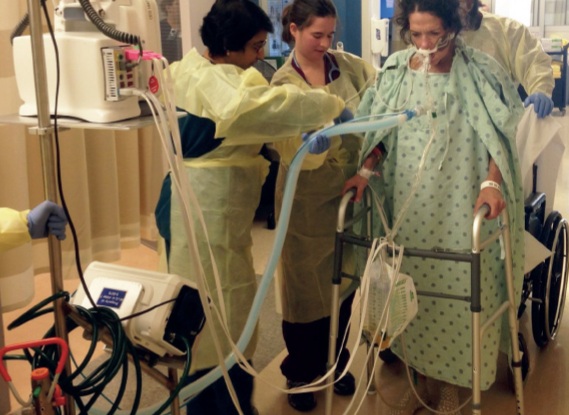
Physical therapy
Before they could send me home, I underwent physical therapy, so I could walk enough to get up the three stairs on my back porch. It was very difficult and painful, as being bed-bound for weeks and the damage the septic shock did to my limbs made it hard to even sit up in bed. Talking was also a struggle as I was intubated for most of my hospital stay and allowed no liquids, so I could only barely manage a whisper for many weeks. It was also very humiliating to be on a diuretic and unable to walk to the restroom, and this caused me a lot of frustration and shame.
By the time it was all over, I had spent a total of 61 days in the hospital. I know that the last eighteen of those days were indescribable for my loved ones. They had stood on the periphery as I fought for my life, not knowing how to make the best decisions for my care. Fear, guilt, anger, and frustration were their only advocates.
Why I tell my story
This is my story, and I tell it because you should know it can happen to anyone, even those that are healthy.
I went into the hospital for a treatable aortic aneurysm. It was a local research hospital where my husband had worked on the university side for years. I was calm and set for surgery. I was confident in my cardiothoracic surgeon and his team. I understood that I would be home in about ten days. It sounds silly now, but my biggest fear was choosing a tissue valve, as I did not want to be on Warfarin for the rest of my life.
Sixty-one days and one contaminated surface later, I left the hospital with an antibiotic-resistant HAI and chronic endocarditis that requires a lifetime of treatment and medical supervision.
As in my case, most HAIs are acquired via contact with contaminated surface materials – medical devices, countertops, bathroom fixtures, etc. Addressing the complex issue of surface contamination is one of the most crucial – yet overlooked – steps in interrupting the transmission of these dangerous, multi-drug-resistant pathogens.
I became a volunteer board member at the Healthcare Surfaces Institute after being invited as the keynote speaker the previous year and telling my patient story. HSI is a group of researchers, infection prevention nurses, medical device manufacturers, and people who create innovations to help prevent infections. This collaboration is very important to me as they understand that a multi-pronged approach to infection prevention is the only way we can tackle this growing problem.
Mary Millard, M.Ed. is a former LPN and serves on the board of the Healthcare Surfaces Institute. As a patient advocate who is living with a chronic healthcare-associated infection, she shares her story to help raise awareness of the devastation that these infections cause and how surfaces play a large part in spreading pathogens in a healthcare setting. More information on her case and speaking history can be found on her website: https://marymillard.org
As a 501(c)(3) non-profit organization, we rely on donations to save lives. We need your help.
Please consider donating, becoming a member, or exploring corporate sponsorship through your workplace today.

