Recalls of Medical Equipment Due to Cleaning Agent Damage Highlight Need for a Call to Action
The Association for Healthcare Value Analysis Professionals (AHVAP) continues to collaborate with the Healthcare Surfaces Institute (HSI) to improve the state of patient care through understanding and continuing to advance the knowledge of the healthcare industry regarding the decision-making process chain from raw materials to finished medical product.
The most recent Covid-19 healthcare crisis has illuminated the fragile nature of the healthcare outcomes ecosystem. In hindsight looking back to pre-2020 with a new set of eyes, we can see where one aspect of the current state began to gather momentum – the rise of super microbes and their effect on the healthcare outcomes ecosystem.
Superbugs and the rise of disinfectants
From the discovery of penicillin in the 1940s to the rapid rise of new natural and synthetic antimicrobial treatments, we have witnessed the evolution of multi-drug resistant (MDR) “superbugs.” Parallel to those events was the need to find alternatives to the common cleaning and disinfection methods of that time, e.g. scrubbing with soap and water or water with additives like bleach.
As the MDR superbugs continued to become more resistant, the cleaning and disinfecting agents became more complex. Major classes of ingredients in different concentrations, such as quaternary ammonium compounds and phenolics, were developed and tested against different microorganisms per EPA guidelines and then classified by their efficacy.
How the disinfectants we use against superbugs help them spread
In the face of MDR superbugs and new disinfectant chemistries, three phenomena occurred. First, the transference of the MDR microorganisms found in the hospital environment to vulnerable patients were labeled as Healthcare-Acquired Infections (HAIs). This led to new Infection Prevention and Control (IP&C) isolation stages to include the type and use of PPE, cleaning and disinfection specifics and timing, and the role of environmental services practices in helping to quell the spread.
The second was the breakdown of surfaces in patient care environments such as countertops, bedrails, flooring, upholstery, mattress covers and ultimately mattresses, and other inanimate surfaces. These have been found to harbor microorganisms linked to HAIs and are hard to clean and disinfect on affected surfaces.
The last and the most misunderstood observation is damage to reusable patient care equipment and accessories. This equipment is either permanently placed in patient care rooms or is part of a fleet of commonly used equipment moved from patient to patient when needed. The damage ranges from faded or obliterated instructional markings to visible abrasions or surface cracks to non-functioning controls with intermittent or permanent damage pre-, during- or post-patient use. Some of these damages occurred several months or years before their published useful life cycle.
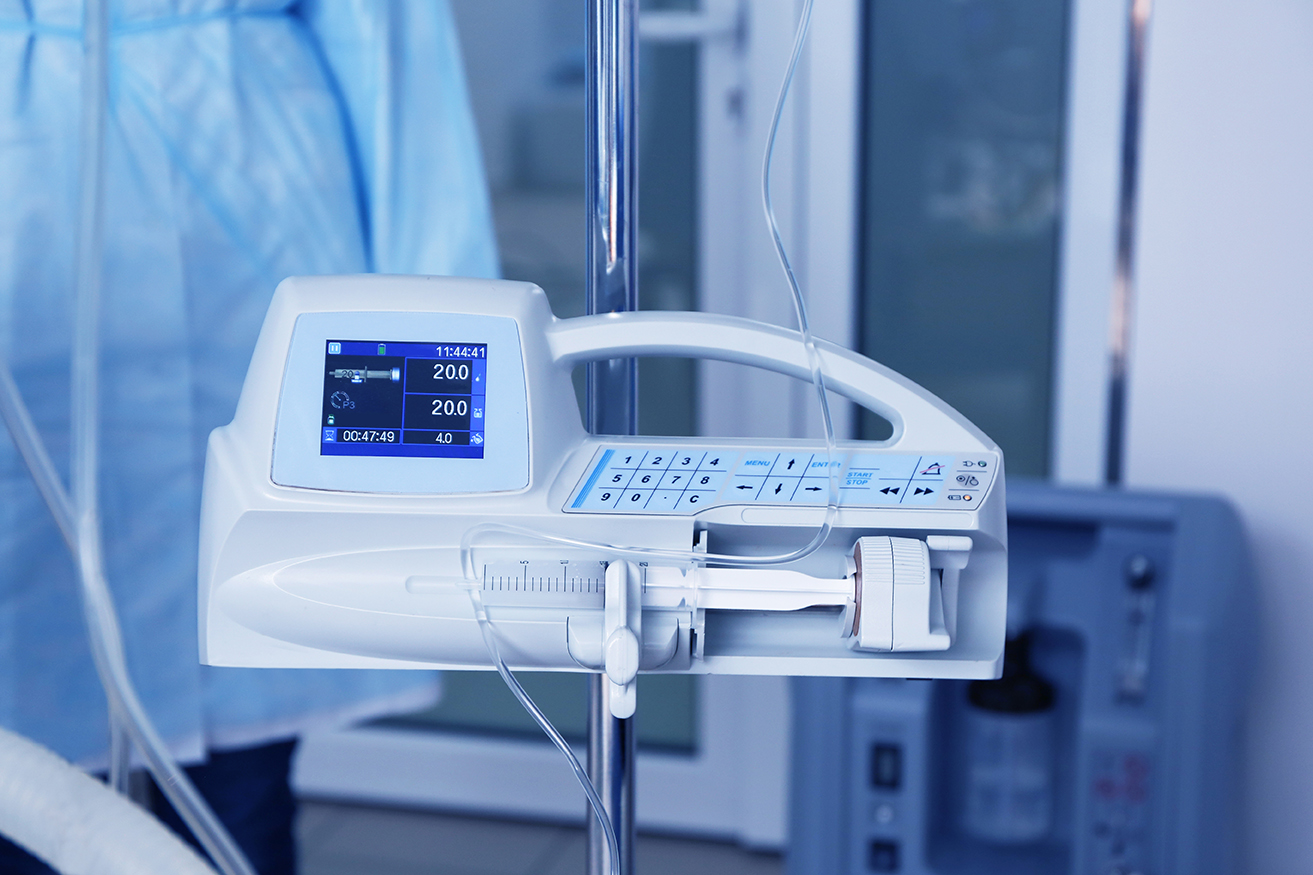
Damaged medical devices get recalled and signal a need for action
Between 2020 and February 2022, three recalls were issued for different manufacturer’s reusable infusion pumps (2- Class I, 1-Class II), and one Class II recall was issued for a disposable infusion pump accessory for reasons related to:
- Cleaning agents may damage connectors which may lead to interruption of communication or power and an interruption of therapy or monitoring
- Update of Instruction For Use (IFU) for safety communication regarding cleaning practices
- Due to cracks, the pump hardware may be damaged by fluid used during the cleaning process
- Cleaning products, containing but not limited to hydrogen peroxide, bleach, alcohol, or antiseptic agents and solvents…may cause damage, such as leaking or cracking
Value Analysis professionals use a process like a checklist to determine the critical elements for any new equipment, product, or service request. By pulling together existing nursing or service line teams, or ad hoc clinical and non-clinical subject matter experts such as Biomedical Engineering, Value Analysis gathers objective clinical, environmental, safety, quality, infection prevention and control, recall reports, service/maintenance records, and other information related to the specific initiative to establish need before costs are factored in.
In the case of reusable, cleanable equipment and accessories, the question asked of manufacturers focuses on the IFUs regarding cleaning and disinfection. IP&C weighs in when the specific wipe or solution containing the class of active chemical ingredient may or may not align with the standard in their healthcare organization. The reason for these discussions is the lack of specificity of language related to how and what the manufacturer uses to comply with testing to inform the IFU.
Based on the real-world experiences that have led to reported recall incidences with root causes attributable to cleaning, disinfectants, and body fluids, a new pause for the cause in purchasing reusable medical equipment and accessories decision-making must occur beginning today.
HSI is bringing together medical device manufacturers, raw materials producers, cleaning and disinfectant firms, IP&C, nursing, biomedical engineers, academics, value analysis, and other professionals to study this issue to stop this deadly threat.
Further Discussion: Read the case study “Surface disinfection incompatibility with medical devices creates potential patient risks” co-released by HSI and AHVAP.
As a 501(c)(3) non-profit organization, we rely on donations to save lives. We need your help.
Please consider donating, becoming a member, or exploring corporate sponsorship through your workplace today.

